Introduction
The oesophagus is also known as the gullet or food pipe. Food passes through the mouth and into the oesophagus before entering the stomach. Acid reflux usually occurs when stomach contents are pushed back up the oesophagus, causing irritation of its lining. This can often occur as a result of a hiatus hernia, where parts of the stomach and sometimes the intestines slide upwards through the diaphragm and into the chest cavity. Hernia repair surgery may be performed alongside the anti-reflux surgery.
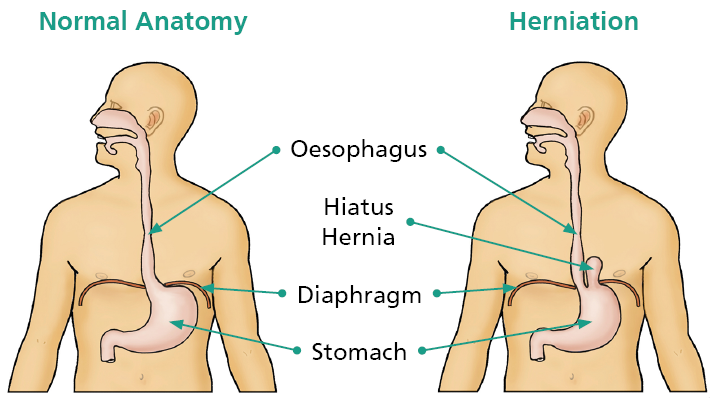
What happens after the surgery?
To allow healing and prevent damage to the surgical site it is important that you follow the dietary advice in this booklet.
Solid foods can put extra pressure on the surgical site, causing discomfort/pain, vomiting and possibly affect your recovery.
For the four weeks after your surgery, you will need to change the type of food you eat. This leaflet explains the changes you will need to make. After four weeks, most patients are able to return to eating normal texture food.
Eating and drinking after surgery
It is normal to feel worried or nervous about eating and drinking after your surgery. After your surgery, you will be allowed to have sips of water only for comfort for the remainder of that day. Unless advised otherwise by your surgeon, you should follow the diet plan below:
- Weeks 1 and 2 – Liquid diet
- Weeks 3 and 4 – Soft/moist diet
- Weeks 5 onwards – Normal textured diet, depending on your progress during the first four weeks
What can I have on a liquid diet (Weeks 1 and 2)?
Build up the amount of liquid you drink little by little over the first few days after surgery to avoid feeling uncomfortable. You are advised to avoid all fizzy drinks as these can make you feel particularly uncomfortable.
To ensure you receive enough energy, protein and other nutrients which are needed for your recovery, liquids should be as nourishing as possible.
Milk
Milk-based drinks are a good option for the first two weeks. Aim for two pints of milk per day. Use full fat (blue top) milk if you can tolerate it. This can be made more nourishing by adding milk powder to it, as follows:
- Pour one pint of full fat milk into a jug
- Add four tablespoons of dried skimmed milk powder
- Stir well with a fork or whisk until the powder is completely blended into the milk
- Keep the jug covered in the fridge and use as needed
If you cannot tolerate cow’s milk, then plant-based milks can be used instead, as long as they are fortified with vitamins and minerals, including calcium (check the bottle to make sure). Speak to your dietitian if you are unsure.
Other fluids
The following are also allowed as part of a;
- Smooth soups (no bits), e.g. cream of chicken, cream of tomato, homemade soups that are blended
- Homemade milkshakes or smoothies
- Shop-bought milkshakes, yoghurt drinks, Lassi, Ayran
- Smooth yoghurts
- Fruit juices
- Still squash/cordial
- Still water
- Teas, coffees, hot chocolate
- Malted milk drinks, e.g. Horlicks, Ovaltine
- Nutritional supplement drinks, e.g. Fortisips, Complan, Scandishake, Nurishment
It is particularly important that you think about how you will get enough protein during weeks one and two when just on liquids.
What can I have on a soft moist diet (Weeks 3 and 4)?
This may also be described as a ”sloppy diet” and includes foods that need minimal chewing and are easy to swallow. The food needs to be mashed or fork-mashable and combined with a sauce or gravy, or simmered in liquid to keep soft.
You should eat a soft moist diet for at least two weeks after the liquid diet stage. This will allow ongoing healing and reduce the risk of damage or re-herniation of the surgical area. It will also help to improve your confidence in eating. Please note, you do not need to eat pureed food or meals. It is difficult to get all the nourishment you need from pureed foods, which may affect your recovery.
It is important that your diet is as balanced as possible. It should include a variety of foods and drinks from different food groups, as shown in the Eatwell Guide below:
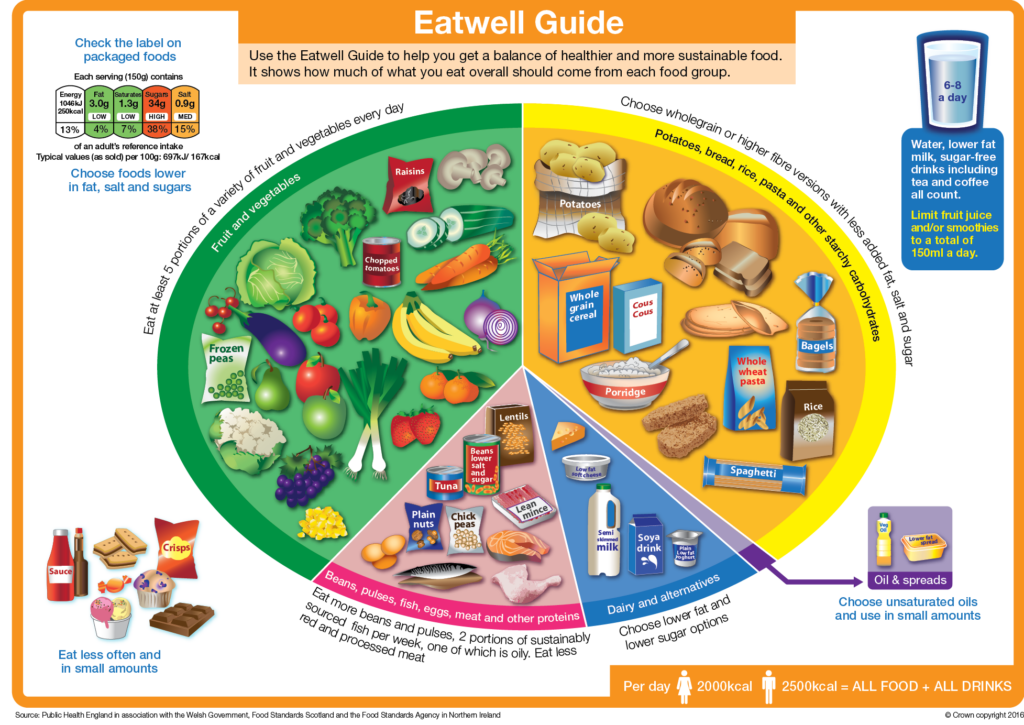
The tables on the next few pages list what soft moist foods are suitable from each of these food groups.
Bread, rice, potatoes, pasta and other starchy foods.
These foods provide energy and B vitamins. Try to include one of these foods at each meal.
Choose
- Porridge, Weetabix or breakfast cereals that soften with plenty of milk
- Mashed potato/sweet potato
- Jacket potato (no skin) with plenty of butter or moist filling
- Pasta, noodles or rice with plenty of smooth sauce
- Polenta, couscous, quinoa
- Yorkshire puddings softened with plenty of gravy
- Pancakes
- Bite and dissolve crisps e.g. corn puffs, Quavers®, Skips®
- Plain cake softened with plenty of custard
Avoid (until week 5)
- Granola, muesli, All Bran
- Potato skins, hard or oven chips
- Deep pan pizza and pizza crusts
- Popcorn
- Potato crisps
Some people find bread difficult to manage initially, this is because it can absorb fluids, swell and may feel like it is sticking.
Meat, fish, eggs, beans and alternatives.
These foods are a good source of protein which helps with the healing process. Try to include protein at least three times per day.
Choose
- Minced chicken, beef, pork, lamb, turkey and soya/vegetarian products and served with gravy or smooth sauce
- Slow cooked stew or casserole. Ensure meat is very tender
- Corned beef
- Meat loaf, meat balls, burger patty or skinless sausages served with a smooth sauce or gravy
- Potted meat or meat paste
- Deli soft sliced meats, e.g. wafer thin ham, chicken, turkey
- Pate
- Soft cooked beans, lentils or dhal
- Chickpeas (if mashed or pureed)
- Dips such as houmous, guacamole, tzatziki or taramasalata
- Smooth nut butters
- Eggs – soft boiled, poached, fried, scrambled or in omelette
Avoid (until week 5)
- Roast meats, steak, chops or tough cuts of meat
- Dried or cured meat
- Crusty pastry
- Nuts and seeds
- Hard boiled eggs
Milk and dairy foods.
These foods provide an important source of protein and calcium to help keep your bones strong. Try to have three servings per day. Choose full fat options where possible.
Choose
- Milk and milk puddings
- Fortified dairy free milk alternatives, e.g. soya milk, oat milk
- Melted or grated cheese
- Cottage cheese
- Yogurts or fromage frais
- Evaporated milk
- Ice cream
- Custard or egg custard (no pastry)
- Rice pudding, tapioca, sago, semolina
Avoid (until week 5)
- Foods that are difficult to swallow or cause discomfort, e.g. hard cheese, cheese with dried fruit or nuts
Fruit and vegetables.
These foods provide essential vitamins, minerals and fibre. Aim to have five portions per day. Ensure firm varieties of fruits and vegetables are well cooked or stewed. Serve with sauce, cream or custard to add extra nourishment.
Choose
- Banana, mango, melon, berries or plums
- Stewed apple, pears, apricots
- Tinned peaches, pears, mandarins
- Fruit juices (sip a small glass/100ml portion slowly)
- Well-cooked, mashed carrots, parsnips, butternut squash, pumpkin, or turnip/swede
- Chopped, tinned tomatoes
- Cooked spinach, courgettes or aubergines
- Avocado
- Well-cooked cauliflower, broccoli with stalks cut short
- Mushy peas, baked beans or soft pulses
Avoid (until week 5)
- Pith e.g. oranges and grapefruit
- Skins e.g. grapes
- Stalks
- Pips and seeds
- Stringy vegetables e.g. celery, green beans or asparagus
- Sweet corn, peas or mushrooms
- Raw vegetables such as onion, peppers, carrots
- Dried fruit
- Fruits such as raw apple or pineapple
To make vegetables soft they need to be well cooked. This means a lot of the nutrients are lost in the cooking water. Use the cooking water to make gravy, stocks or sauces. You may wish to discuss with your dietitian about taking a multi-vitamin and mineral supplement.
Meal Ideas
- Shepherd’s or cottage pie with carrot and swede mash
- Fish pie topped with fortified mashed potato
- Moussaka
- Lasagne, macaroni cheese, cannelloni, ravioli
- Chilli con carne and rice
- Slow cooked curries (soft meat) and rice
- Lentil dahl
- Congee
- Slow cooked stew or casserole
- Corned beef hash
- Omelette made with extra butter and cheese
- Beans on toast (without crusts) with cheese
- Inside of jacket potato with beans, cheese, tuna mayonnaise
What changes should I make to the way I eat?
Initially, you may be unable to eat the portion sizes you managed before your operation. You may feel full very quickly.
- Aim to follow a little and often meal pattern, e.g. six small meals per day or eating every 2 – 3 hours.
- Take your time, eat slowly and ensure you chew foods well.
- Separate food and liquids. Avoid drinking 30 minutes before eating and 30 minutes after, to avoid overfilling.
- Sitting up straight, ideally in a chair, when eating can help food to pass more easily into your stomach. Try to remain upright for 30 minutes after eating.
- Make sure you have some protein foods daily to avoid loss of lean muscle mass (see sections above on ‘meat, fish, egg…’ and ‘milk and dairy foods’).
Enriching your food
It is useful to enrich your diet in the first four weeks following your surgery to improve its energy and protein content. This can help maintain your weight or promote weight gain if necessary.
Ways to enrich a liquid diet:
- Use fortified milk (as described earlier) to make milky drinks e.g. coffee, hot chocolate or malted drinks such as Ovaltine or Horlicks.
- Add butter, oil, cream, crème fraîche or grated cheese to soups or liquidised meals
Ways to enrich a soft moist diet:
- Use fortified milk (see page 4) to make milky drinks e.g. coffees, hot chocolate, malted drinks like Ovaltine ® or Horlicks ®
- Add butter, oil, cream, crème fraîche or grated cheese to soups
- Add cream, crème fraiche, yoghurt or soft ice cream to milkshakes or smoothies
- Melt cheese on scrambled eggs, baked beans, pasta dishes, shepherds’ pie or fish pie
- Add butter or spread to softened vegetables, mashed potatoes or eggs
- Use fortified milk to make sauces, custards or other milky puddings and to pour on breakfast cereal
- Use generous amounts of butter or oil when cooking
- Add grated cheese and/or butter to mashed potatoes, softened vegetables or sauces
- Add an extra egg to any suitable dishes such as a carbonara sauce
- Add evaporated milk, cream or crème fraîche to sweet or savoury foods including soup, curry, casseroles, porridge, fruit or milky puddings
Week 5 onwards – Returning to normal texture food
If you had no issues during the two weeks of soft moist foods, you can gradually reintroduce normal textures again. However, the amounts of food you are able to eat may remain smaller for a while longer.
A small amount of weight loss is likely after surgery while you build up your diet. If it is more than 7lbs/3.5kg and you are concerned, please inform your surgeon.
Do I need to avoid alcohol?
Following this surgery, alcohol is allowed within weekly recommended limits. This is set at no more than 14 units of alcohol per week for both men and women. For further information on alcohol advice, please see:
www.nhs.uk/live-well/alcohol-advice/
Please be aware that lager and other fizzy drinks may make you feel uncomfortable, so you should avoid these. Also, large volumes of liquid, including alcohol, may make you feel full and cause you to eat less.
Personal Notes
You may find it helpful to write down any questions you might have:
If you have any queries please contact
Dietitian:
Contact No: